Central Retinal Vein Problems Treated
Central retinal vein occlusion is the closure of the final retinal vein (located at the optic nerve) which collects all of the blood after it passes through the capillaries. The systemic risk factors for branch retinal vein occlusion mentioned above are also risk factors for central retinal vein occlusion.
Central retinal vein occlusion is generally categorized into two forms: non–ischemic and ischemic. This means that some central retinal vein occlusions are associated with significant obstruction of capillaries or non–perfusion. This predisposes to a peculiar type of neovascularization that occurs in front of the eye on the iris (rubeosis irides). These eyes may develop a very high pressure known as neovascular glaucoma due to obstruction of the fluid outflow channels. This is a very serious complication which is associated with severe vision loss and may cause pain and loss of the eye itself. Laser photocoagulation treatment is very useful in managing rubeosis irides. If performed early in the course (when iris neovascularization is first detected), it may help prevent these complications. Patients with recent central retinal vein occlusions must be followed frequently in order to detect this complication in a timely manner.
Less frequently than in branch vein occlusion, patients with central retinal vein occlusion may also develop neovascularization in the back of the eye, causing vitreous hemorrhage and retinal detachment. Laser treatment may be useful in managing these complications.
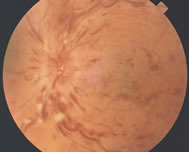
This is a color photograph showing diffuse intraretinal hemorrhage of a central retinal vein occlusion.
As with branch retinal vein occlusion, macular edema, and non–perfusion is also frequently seen with central retinal vein occlusion. Macular edema, even without significant macular ischemia, is not treated routinely with laser photocoagulation. This is because a recent study failed to show a benefit for patients with central retinal vein occlusion, particularly for those who are elderly. (In contrast, laser treatment has been shown to be effective for patients with branch retinal vein occlusion). It is possible, but not proven, that some young patients with central vein occlusion of the non–ischemic type may benefit from localized laser treatment for macular edema.
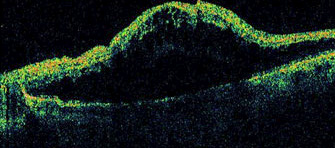
Optical Coherence Tomography showing macular edema from a central vein occlusion.
Some patients with macular edema from central vein occlusions may respond to the off-label intraocular injection of steroids (triamcinolone) or anti–vasogenic drugs (Avastin). These pharmacologic agents wear off over a period of approximately two months and may need to be re-injected if the edema returns. Optical Coherence Tomography (OCT) is a useful test for the detection of macular edema in CRVO and for following the response to treatment.
If the fluorescein angiogram indicates that capillary non–perfusion is the cause of the vision loss, it is unlikely that the vision will improve significantly over time regardless of any treatment.
If a patient develops an occlusion of the central vein in both eyes, there is a greater possibility of an underlying systemic cause. It is recommended (by our group) that such patients have a thorough medical workup as outlined previously.
Sometimes in venous occlusive disease, scar tissue can form on the surface of the retina. This condition, which is called a macular pucker or an epiretinal membrane, may result in distorted vision (metamorphopsia) which is not improved with laser or pharmacologic treatment. Vitrectomy surgery may be indicated for the removal of a macular pucker.
The most devastating potential problem in a vein occlusion is that of neovascularization. The neovascularization may develop in 40% of those cases where branch vein occlusions produce large areas of capillary non–perfusion. This retinal neovascularization generally develops in the first 6 to 12 months after the occlusion. Unless laser treatment is performed, at least 60% of the patients with neovascularization will experience episodes of vitreous hemorrhage. In severe cases of neovascularization, retinal detachment can occur from pulling by these vessels and associated scar tissue on the retina (traction detachment).
Laser photocoagulation treatment is a proven therapy for neovascularization in vein occlusions. Indeed, laser treatment can cause stabilization or, at times, regression of vascular growth. This treatment, while important in helping to prevent further visual loss, is not usually associated with improvement in vision. As vein occlusions evolve, some normal vessels may dilate to compensate for the obstructed vein. Sometimes, these collateral vessels may be difficult to distinguish from neovascularization on clinical examination. A fluorescein angiogram may be useful in this determination.
Recently, the intraocular injection of anti–vasogenic drugs, that tell blood vessels to stop growing, has shown promising results in the control of retinal neovascularization. These treatments have not yet been assessed in prospective clinical trials but may be used on an off-label basis. One particular medication that has been increasingly utilized for this purpose is Avastin, a drug that is approved for the intravenous treatment of colon cancer. Intraocular injections of Avastin have shown promising early results, and an excellent safety profile, in the control of retinal swelling and neovascularization due to a variety of retinal conditions. Avastin lasts about 6 weeks in the eye after a single injection and may need to be repeated if the disease reactivates. Although eye injections may sound painful, they are simple to perform, relatively painless, and well-tolerated by patients.
In summary, retinal vein occlusions develop from obstruction of the venous outflow from the eye. The blockage may vary in size and location, accounting for a wide range of retinal outcomes. Some of the complications of retinal vein occlusion may be appropriately managed with laser treatment. It is hoped that through further research, even better strategies for prevention and management will be developed.
Eye Center of Texas is an established eye care practice led by experienced LASIK surgeons Dr. Wade and Dr. Mayo. Using the latest laser technology and surgical techniques, they have helped many patients regain their vision and enhance their quality of life. In addition to LASIK, Eye Center of Texas is also frequently visited by patients searching for a qualified cataract surgeon in Houston.
Financing Options Available
Apply today to find a financing option that meets your needs.
Our Locations
Houston/Bellaire
6565 W. Loop S., Suite 650Bellaire, TX 77401
Medical Office:
713-797-1010
Medical Fax:
713-357-7276
LASIK/Near Vision:
Office: 713-395-1515
Fax: 713-357-7278
Pasadena
4415 Crenshaw RoadPasadena, TX 77504
Medical Office:
281-977-8800
Medical Fax:
281-977-8877
Sugar Land
15400 S.W. Freeway, Suite 301Sugar Land, TX 77478
Medical Office:
281-277-1010
Medical Fax:
281-277-4504
Clear Lake
455 E. Medical Center Blvd., Suite 110Webster, TX 77598
Medical Office:
281-332-1397
Medical Fax:
281-282-9152
Katy
Greenhouse Medical Plaza2051 Greenhouse Road, Suite 110
Houston, TX 77084
Medical Office:
713-797-1010
Medical Fax:
713-357-7276
The Woodlands/Conroe
100 Medical Center Blvd., Suite 118Conroe, TX 77304
Medical Office:
713-797-1010
Medical Fax:
936-647-1620