Treating Retinal Conditions
- Retinal Artery Occlusion
- Choroidal Nevus
- Choroidal Neovascular Membrane (CNVM)
- Cystoid Macular Edema
- Ocular Histoplasmosis Syndrome
- Retinitis Pigmentosa
- Stargardt’s Disease
- Temporal Arteritis (Giant Cell Arteritis)
- Uveitis
Retinal Artery Occlusion
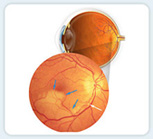
A retinal artery occlusion occurs when the central retinal artery or one of the arteries that branch off of it becomes blocked. This blockage is usually caused by a tiny embolus (blood clot) in the bloodstream. The occlusion decreases the oxygen supply to the area of the retina (i.e., a retinal “stroke”) nourished by the affected artery, resulting in permanent vision loss.
The following conditions increase your risk of retinal artery occlusion:
- High cholesterol
- Heart disease
- Arteriosclerosis
- Hypertension
- Diabetes
- Glaucoma
Signs and Symptoms
*Sudden, painless, loss of vision in one eye (complete loss of vision for central artery occlusion, partial loss of vision for branch artery occlusion.)
Treatment
Unfortunately, there is no treatment that can consistently restore vision lost from an artery occlusion. However, if the problem is caught within the first hour and treatment begins immediately, partial recovery may be occasionally possible.
Choroidal Nevus
A nevus is a flat, benign, pigmented area that may appear inside the eye or on its surface. Nevi commonly appear on the choroid, the iris, and the conjunctiva. They are similar to freckles and don’t typically change shape or grow.
Signs and Symptoms
- Brownish, freckle-like spot
- Usually flat
Treatment
Though most nevi are harmless, they should be monitored for changes. Your doctor may take photos or use ultrasound to document the size, shape, and other characteristics of the nevus. In rare cases, the nevus may be biopsied and examined for melanoma (cancer) cells.
Cystoid Macular Edema
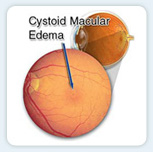
Cystoid macular edema (CME), or swelling of the macula, can occur as a result of disease, injury, or, occasionally, eye surgery. With CME, fluid collects within the layers of the macula, causing blurred, distorted central vision. Though this eye condition rarely causes a permanent loss of vision, recovery is often a slow, gradual process. Most patients recover in two to 15 months.
Signs and Symptoms
- Blurred central vision
- Distorted vision (straight lines may appear wavy)
- Vision is tinted pink
- Light sensitivity
CME Treatment
Many cases of CME can be treated with anti-inflammatory drops. Occasionally, medication is injected near the back of the eye for a more concentrated effect. Oral medications are sometimes prescribed to reduce swelling.
Ocular Histoplasmosis Syndrome
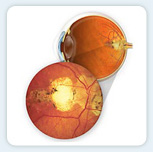
Histoplasmosis is caused by a fungus commonly found in the dust and soil of the Mississippi-Ohio River Valley region. About 62 percent of all adults living in this region are carriers of the syndrome. Men and women are equally affected.
Histoplasmosis is contracted by inhaling dust that carries the fungal spores. The effect of the syndrome on the body varies greatly from one person to another. Many carriers have no symptoms at all, while others experience flu-like symptoms and mild respiratory infections. People who already have a weakened immune system are more likely to be seriously affected by histoplasmosis.
The fungus can affect the eye by causing small areas of inflammation and scarring of the retina. These are called “histo spots” and can occur in both eyes. The effect of histo spots on vision depends on their location. Spots in the peripheral area of the retina may have little or no impact on vision, while those located in the center of the macula may cause prominent blind spots.
Most people with histo spots in the retina are completely unaware of their presence unless the central vision is affected. Studies indicate that only about 5 percent of people with histo spots are at risk of losing vision.
Signs and Symptoms
- Many patients with histo spots have no symptoms. Others may experience the following:
- Distorted vision
- Blind spots
- Scars in the retina, ranging in severity
Histoplasmosis Treatment
Often, ocular histoplasmosis does not require any treatment. If you are diagnosed with this condition, your doctor will probably recommend that you closely monitor your central vision with an Amsler grid. When the condition causes abnormal blood vessels to develop in the central retina, laser eye surgery may be used. In some cases, surgical removal of the tiny, abnormal vessels has been successful.
Retinitis Pigmentosa
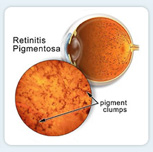
Retinitis pigmentosa (RP) is a rare, hereditary disease that causes the rod photoreceptors in the retina to gradually deteriorate. The rods are located at the edge of the retina and are responsible for peripheral and night vision.
People with RP usually first notice difficulty seeing in dim lighting and gradually lose peripheral vision. The effect this disease has on vision can range from mild problems to blindness.
RP affects males more than females. Though it is frequently diagnosed during childhood, some people do not have noticeable symptoms until later in life.
Signs and Symptoms
- Difficulty seeing in dim lighting
- Tendency to trip easily or bump into objects when in poor lighting
- Gradual loss of peripheral vision
- Glare
- Loss of contrast sensitivity
- Eye fatigue (from straining to see)
Retinitis Pigmentosa Treatment
Currently, there is no standard retinitis pigmentosa treatment or therapy available to patients at our practice. However, Vitamin A palmitate has been found to slow down progression, and researchers are studying possible treatment options such as retinal implants and drug therapy. Work is also being done to isolate the genes that are responsible for the disease.
Stargardt’s Disease
Stargardt’s disease (also known as fundus flavimaculatus) is a type of macular degeneration that typically surfaces before the age of 20. This disease is an inherited disorder that causes a progressive loss of central vision of both eyes but does not affect peripheral vision.
Signs and Symptoms
Stargardt’s is a progressive disease. Symptoms may be mild at first, but will usually worsen over time. Early symptoms include the following:
- Blurred vision not correctable with glasses or contact lenses (this is one of the earliest symptoms)
- Difficulty adapting from bright sunlight to a dimmer room
- Later symptoms
- Progressive deterioration of central vision
- Missing areas of central vision
- Central blind spot
- Diminishing ability to perceive colors
Treatment for Stargardt’s
Unfortunately, there is no known cure for Stargardt’s.
Temporal Arteritis (Giant Cell Arteritis)
Temporal arteritis, also known as giant cell arteritis, is an inflammatory condition that affects the medium-sized blood vessels that supply the head, eyes, and optic nerves. Patients with temporal arteritis experience swelling and tenderness in the blood vessel of the temple and scalp. The disease is most common in people over age 60 and affects women about four times more than it affects men. If allowed to progress, temporal arteritis can be sight threatening. Vision loss occurs when the inflamed arteries obstruct blood flow to the eyes and optic nerves. Temporal arteritis may also start to affect arteries in other areas of the body. Prompt treatment of this condition is essential to prevent permanent vision loss and other health problems.
Signs and Symptoms
Patients with temporal arteritis usually notice visual symptoms in one eye at first, but many notice symptoms in the fellow eye within days if the condition is untreated. The following are some of the most common warning signs of the condition:
- Headache
- Loss of appetite
- Fever
- Fatigue
- Depression
- Drooping lid
- Double vision
- Sore neck
- Tenderness of scalp (combing hair may be painful)
- Pain in temple area (may be excruciating)
- Transient blurred vision
- Jaw soreness, especially when chewing food
Treatment
The ophthalmologist often works in conjunction with the patient’s internist to treat this disease. The primary treatment is oral steroid medication to reduce inflammation. Most patients notice an improvement in their symptoms within several days of receiving treatment. In some cases, long-term steroid use is necessary.
Uveitis
Uveitis is a general term that refers to inflammation or swelling of the structures of the eye that are responsible for its blood supply. These structures are collectively known as the uveal tract and include the iris, ciliary body, and choroid. Uveitis is often caused by infection or underlying disease, but sometimes the cause is unknown. The condition usually affects people between 20 and 50 years of age.
Forms of Uveitis
There are four main categories of uveitis:
- Anterior Uveitis (also known as Iritis) – involves the iris and ciliary body and is the most common type
- Intermediate Uveitis – affects the ciliary body, vitreous, and retina
- Posterior Uveitis – involves the retina, choroid, and optic nerve
- Diffuse Uveitis – affects structures both in the front and back of the eye
Signs and Symptoms
Anterior
- Light sensitivity
- Blurred vision
- Elevated intraocular pressure
- Small pupil
- Tearing
- Redness around the iris
- Pain that may range from aching or soreness to intense discomfort
Intermediate
- Often affects both eyes
- Floaters
- Blurred vision
Posterior
- Blurred vision
- Pain (if the optic nerve is involved)
Diffuse
- Combination of symptoms from anterior, intermediate, and posterior uveitis
Uveitis Treatment
The appropriate treatment for uveitis is dependent on the severity of the disease and the ocular structures involved. Topical eye drops and/or oral medications may be prescribed to reduce inflammation. In some cases, medication is required to reduce intraocular pressure. After inflammation has subsided, treatment may be required for secondary conditions such as cataracts, glaucoma, or the presence of scar tissue.
Strabismus
Eye Center of Texas is an established eye care practice that is equipped with state-of-the-art technology to help patients obtain their best vision. Led by Dr. Wade and Dr. Mayo, the practice is frequently visited by patients searching for an experienced Houston cataract surgeon or LASIK surgeon. With five locations throughout Texas, the practice is a leader in refractive surgery throughout Houston, Pasadena, Clear Lake, Katy and Sugar Land, TX.
Financing Options Available
Apply today to find a financing option that meets your needs.
Our Locations
Houston/Bellaire
6565 W. Loop S., Suite 650Bellaire, TX 77401
Medical Office:
713-797-1010
Medical Fax:
713-357-7276
LASIK/Near Vision:
Office: 713-395-1515
Fax: 713-357-7278
Pasadena
4415 Crenshaw RoadPasadena, TX 77504
Medical Office:
281-977-8800
Medical Fax:
281-977-8877
Sugar Land
15200 S.W. Freeway, Suite 130Sugar Land, TX 77478
Medical Office:
281-277-1010
Medical Fax:
281-277-4504
Clear Lake
455 E. Medical Center Blvd., Suite 110Webster, TX 77598
Medical Office:
281-332-1397
Medical Fax:
281-282-9152
Katy
Greenhouse Medical Plaza2051 Greenhouse Road, Suite 110
Houston, TX 77084
Medical Office:
346-547-7070
Medical Fax:
281-214-2971
The Woodlands/Conroe
100 Medical Center Blvd., Suite 118Conroe, TX 77304
Medical Office:
936-647-1610
Medical Fax:
936-647-1620
Cypress
22215 Cypresswood Dr., Suite 116Cypress, TX 77433
Main Phone:
(346) 537-0088
Fax Line:
(346) 537-0187