Retinal Tear Surgery & Retinal Detachment Surgery
What you should know about retinal detachment
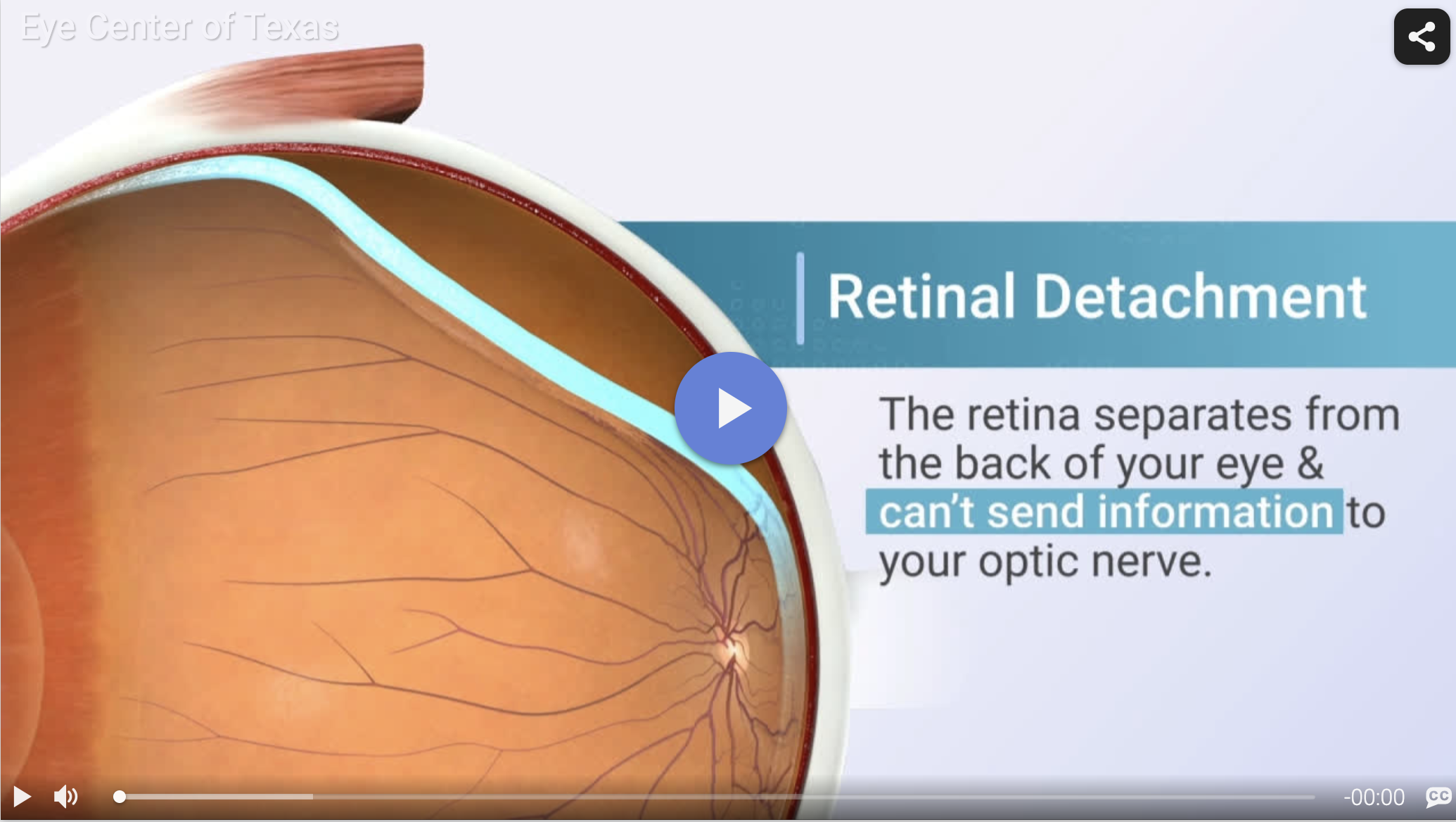
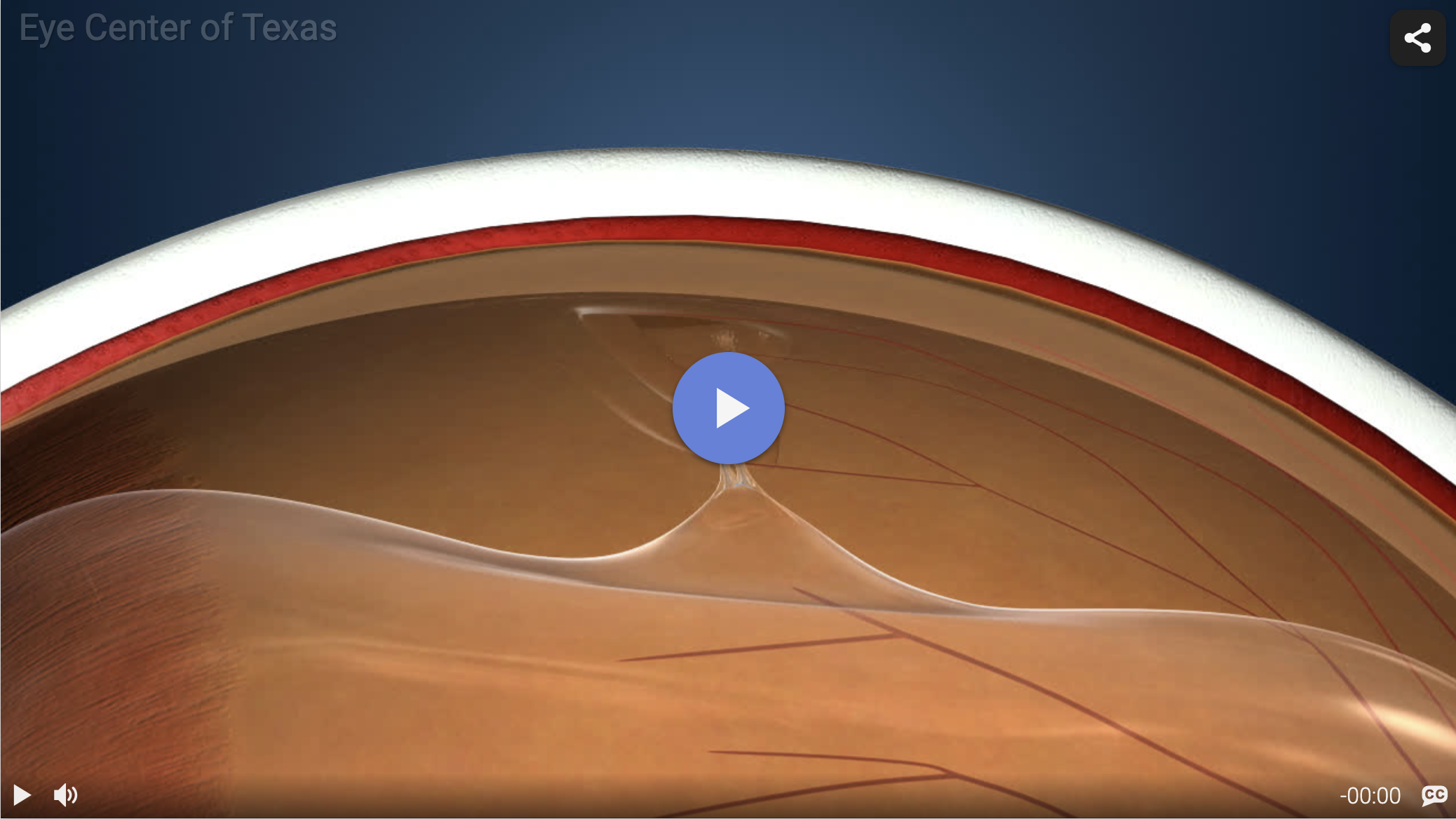
The neurosensory tissue lining the back wall of the eye is known as the retina. It functions something like the film in a camera, and its main role involves creating the images that one’s mind and eyes see. When the retina detaches, it separates from the back wall of the eye, thus removing it from the blood supply and nutrition it needs to function.
The retina will degenerate and lose its ability to function over time if it remains detached, so retinal tear surgery is required to restore proper sight. Knowing the symptoms of a retinal tear and when to see an ophthalmologist for retinal tear laser surgery make all the difference in determining the quality of the results as well as the length of time it will take to recover.
If you’re looking for an ophthalmologist in Houston to assist with eye conditions, including retinal detachment, the specialists at Eye Center of Texas know what to do to ensure a strong recovery.
Symptoms of retinal tears
Early detection is key in successfully treating retinal detachments and tears. Awareness of the quality of your vision in each eye is extremely important, especially if you have a medical condition that increases your risk, such as nearsightedness or diabetes. Compare your vision daily by looking straight ahead and covering one eye, then the other.
Notify your doctor immediately if you notice any of the following:
- Obstruction of your peripheral vision (veil, shadow, or curtain)
- A sudden shower of floaters that resemble spots, bugs, or spider webs
- Light flashes
- “Wavy” or “watery” vision
- A sudden decrease in vision quality
Anyone who has sudden flashes, floaters, or peripheral vision loss needs an urgent examination by an eye doctor familiar with retinal diseases. A careful examination is necessary to diagnose retinal breaks or detachment.
How serious is retinal tear surgery?
Vision loss can progress rapidly. If left untreated, retinal detachment may cause permanent blindness. In most cases, retinal tear laser surgery is scheduled a day or two after a formal diagnosis to preserve the patient’s vision quality as much as possible.
Is retinal tear surgery painful?
Patients receive a local anesthetic when undergoing retinal tear surgery, so they will not feel anything while undergoing the procedure. At most, they may experience a little pressure from time to time.
Are you awake during retinal tear surgery?
As an outpatient procedure, retinal tear surgery is almost always performed while the patient is awake. Depending on the type of procedure they’re undergoing, it can take anywhere from ten minutes to two hours to complete.
Patients who have undergone any type of retinal tear surgery must not drive themselves from the facilities due to their vision being compromised by healing and the aftereffects of anesthesia. It is highly advised to bring a family member or friend along rather than relying on public transportation, taxi, or rideshare service in the event of post-surgical complications arising on the ride home.
What can I expect after laser surgery for a torn retina?
What to expect after laser surgery for a retinal tear depends on the patient’s eyesight prior to receiving surgery. If the patient’s vision is initially good, successful surgery generally yields good results. However, if their overall eyesight is poor before the operation, the patient’s final vision results often decrease even with successful retinal reattachment.
Patients usually need to have their glasses changed out several months after retinal reattachment surgery. Their resulting postoperative vision may also decrease if they develop cataracts, which is a possible side effect of some retinal procedures. Additional cataract surgery may be required to fully restore the patient’s vision.
How long does it take to recover from retinal tear surgery?
The length of a detached retina surgery recovery hinges on a number of factors, including a patient’s age and overall health. It typically takes between 10 days to four weeks to fully recover, during which time the patient may be required to do the following:
- Refrain from driving or operating heavy machinery
- Wear an eyepatch
- Use eye drops
- Rest, sometimes in a particular position
- Refrain from taking certain medications, especially blood thinners and aspirin
Every patient is different. Speak to your ophthalmologist about what your personalized recovery and treatment plan will look like before scheduling your surgery.
Side effects of retinal tear laser surgery
It’s normal to experience some side effects while recovering from retinal tear laser surgery. Depending on your circumstances, your side effects may include the following:
- Flashes or floaters that go away on their own over time
- Blurred vision
- Reduced night vision
- Haloing effects around lights
- Blind spots
- Mild vision loss
- Problems focusing the eyes
- Cataracts, in extreme cases
While these side effects are normal, it’s still crucial to stay in touch with your ophthalmologist if they worsen over time, do not go away after your recovery window has passed, or are so severe they cannot go ignored.
Need more information on retinal tear surgery? Eye Center of Texas can help.
Patients seeking retinal tear surgery have access to all the latest available treatments at Eye Center of Texas. Our team of specialists is experienced in providing retinal tear laser surgery and other procedures meant to help prevent blindness. To schedule an appointment with a retina specialist in Houston, please contact us today. Your eye health can’t wait.
Financing Options Available
Apply today to find a financing option that meets your needs.
Our Locations
Houston/Bellaire
6565 W. Loop S., Suite 650Bellaire, TX 77401
Medical Office:
713-797-1010
Medical Fax:
713-357-7276
LASIK/Near Vision:
Office: 713-395-1515
Fax: 713-357-7278
Pasadena
4415 Crenshaw RoadPasadena, TX 77504
Medical Office:
281-977-8800
Medical Fax:
281-977-8877
Sugar Land
15200 S.W. Freeway, Suite 130Sugar Land, TX 77478
Medical Office:
281-277-1010
Medical Fax:
281-277-4504
Clear Lake
455 E. Medical Center Blvd., Suite 110Webster, TX 77598
Medical Office:
281-332-1397
Medical Fax:
281-282-9152
Katy
Greenhouse Medical Plaza2051 Greenhouse Road, Suite 110
Houston, TX 77084
Medical Office:
346-547-7070
Medical Fax:
281-214-2971
The Woodlands/Conroe
100 Medical Center Blvd., Suite 118Conroe, TX 77304
Medical Office:
936-647-1610
Medical Fax:
936-647-1620
Cypress
22215 Cypresswood Dr., Suite 116Cypress, TX 77433
Main Phone:
(346) 537-0088
Fax Line:
(346) 537-0187